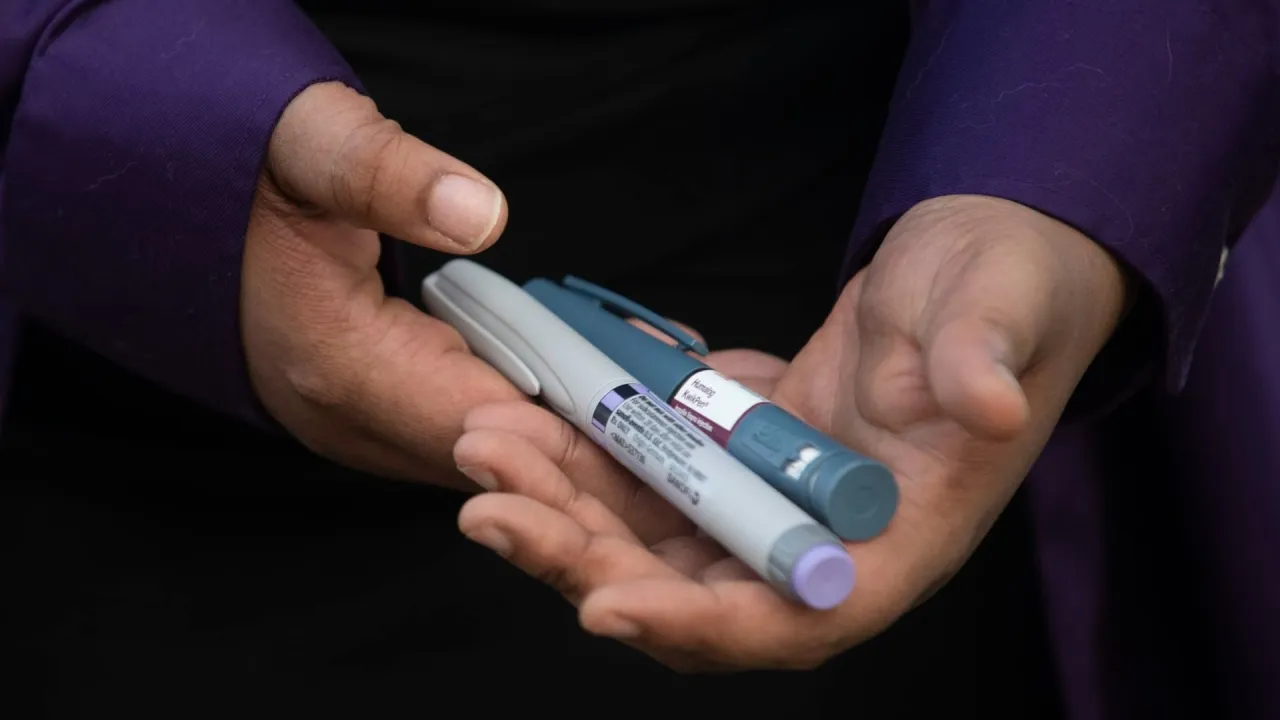
Khaberni - When you have diabetes, you may need to use medication to manage your condition. Sometimes, your doctor may prescribe insulin to regulate blood glucose levels. Depending on your situation, the doctor may use one or more types of insulin to maintain blood glucose levels within the normal range.
For example, according to a report by "healthline," rapid-acting mealtime insulin types are taken just before meals to help control the blood glucose spikes that occur upon eating. The doctor may prescribe mealtime insulin to be taken in addition to long-acting insulin, helping to maintain stable blood glucose levels between meals.
The amount and type of insulin vary from person to person, depending on diet, lifestyle, and your specific condition.
Mealtime insulin versus other types of insulin
The action of mealtime insulin differs from other types, and the main difference between various insulin types lies in how quickly it begins to work in the blood (onset), the time it reaches its peak effectiveness (peak time), and its duration of action (duration).
Rapid-acting mealtime insulin, sometimes called bolus insulin, is designed to quickly impact blood sugar levels during meal consumption. This type of insulin starts working within 15 minutes, reaches its peak about an hour to two hours after injection, and lasts for approximately 3 hours.
The action of regular insulin (short-acting) begins 30 minutes after injection, peaks between two and three hours after injection, and lasts between 3 and 6 hours.
Long-acting insulin, also called basal or background insulin, works in your body all day to control blood sugar levels, even when you are not eating. It typically starts working a few hours after injection and continues for up to 24 hours.
Intermediate-acting insulin is similar to long-acting insulin, but its effect does not last as long; it reaches the bloodstream within 2 to 4 hours after injection and lasts for about 12 to 18 hours.
The effect of very long-acting insulin starts within 6 hours, and because it does not peak, its effect may last for more than 36 hours.
Benefits of mealtime insulin
The greatest benefit of taking mealtime insulin along with long or intermediate-acting systems is that it allows you to align the way your body secretes insulin naturally if it is able to do so.
Another advantage is that it allows flexibility in meal times as long as you remember to take mealtime insulin 15 to 20 minutes before your meal or snack, you can eat your meals whenever you like.
How to determine if mealtime insulin is suitable for you?
Many doctors start by prescribing long-acting insulin initially, but sometimes, long-acting insulin is not sufficient to maintain blood sugar levels at the desired level throughout the day.
When eating a meal, blood glucose levels can rise quickly, and this "spike" in blood sugar may be too high for long-acting insulin to control. In this case, the doctor might want to add mealtime insulin to your long-acting treatment, or prescribe a combined insulin.
You will continue to take long-acting insulin as directed by your doctor, but you will also take mealtime insulin just before your meals (such as before breakfast, lunch, dinner, or having a large snack).
The best times to take mealtime insulin
When you start taking insulin, your doctor may check up on you regularly, and they might ask you to adjust the amount or timing based on blood test results. You might need to adjust your dosage and schedule until you find the most suitable dose for you.
Research suggests that the best time to take insulin is 15 to 20 minutes before the meal, as taking insulin post-meal may increase the risk of hypoglycemia or low blood sugar.
However, there's no need to worry if you forget to take insulin before the meal. Take it at the end of the meal and monitor your blood sugar level.
If you forget to take insulin and it's time for another meal, your blood sugar level will likely be higher than normal before the meal. In this case, measure your blood sugar level then adjust it with the meal, adding a correction dose to cover the high glucose level. Talk to your doctor about how to use the correction dose to control high blood sugar when you forget a dose.